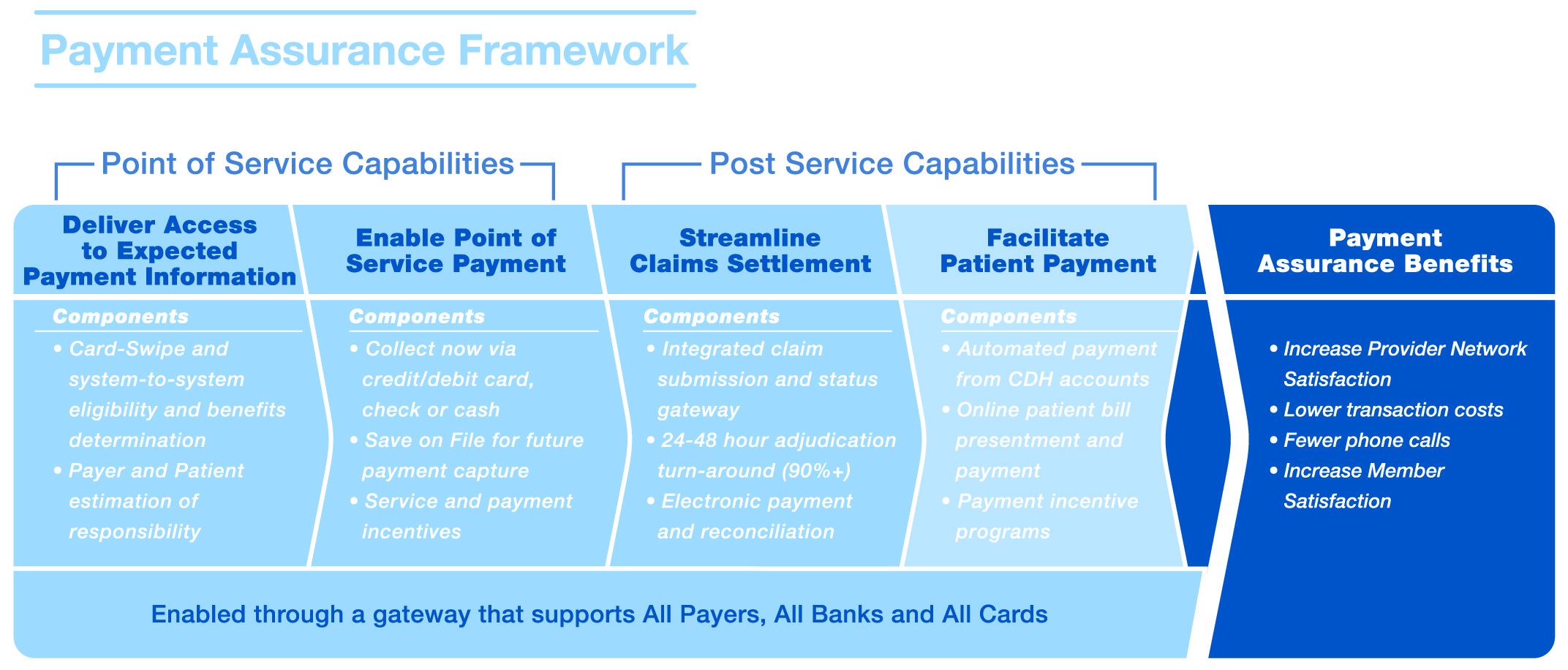
In an earlier post, we discussed one of the major threats to the payer-provider relationship: the provider’s lack of payment assurance. This threat poses an opportunity to payers to give their provider networks the tools needed to achieve payment assurance. In our previous post, we gave tips for payers to deliver payment assurance to their providers. Below, we’ve included a graphic of the Payment Assurance Framework to demonstrate how payers can deliver payment assurance to providers in each step of the healthcare payments process:
Payment Assurance in 5 Steps:
1. Provider front office staff swipes member card at check-in to generate real-time eligibility verification transaction to payer — resulting in pre-authorization of eligibility and member payment responsibility for the appropriate handling by the provider.
2. After services are rendered, provider back office generates claim transaction to payer through the practice management system to the gateway, which routes to the appropriate payer.
Tip: Using a clearinghouse that only processes claim and remittance data is not enough. The most secure and efficient way to manage healthcare payments is by using one system for all healthcare and payment transactions.
3. Payer processes claim and delivers EOP and payer portion of payment to provider electronically.
4. Remaining member payment responsibility is either automatically funded to provider, or presented to member electronically for payment authorization and funding to provider.
Tip: Enable members to pay at all interaction points, including when the explanation of benefits (EOB) is presented. One option is to offer members an easy way to pay online through the payer’s website.
5. Provider receives payer and member payments and automatically reconciles EOP to payer and member payments.
