A decade ago, the consumer’s role in the healthcare decision-making process was drastically different. Payers and employers managed virtually all of the health benefit decisions for consumers. Consumers were presented with one or two choices for a benefits package, visited the providers in their network and paid a minimal copay, if anything at all. Payment associated with healthcare services generally was not a focal point for consumers.
In recent years, the payment responsibility has shifted (and continues to shift) to the consumer. This changing landscape has forced consumers to become decision-makers in the healthcare industry. Indeed, consumers now face a wide variety of health plans to choose from, and they have become sensitive to the costs associated with healthcare, for both consumer-to-provider and consumer-to-payer payments.
As a result, payers and providers need to focus on the consumer experience now more than ever before.
Consumer Expectations
As consumer payments represent a growing portion of provider revenue, providers must meet consumer payment expectations set by other industries, such as offering convenient payment options and the ability to manage payments online.
However, consumers are confused by the disjointed healthcare payments process. For example, examine the consumer experience after a provider visit:
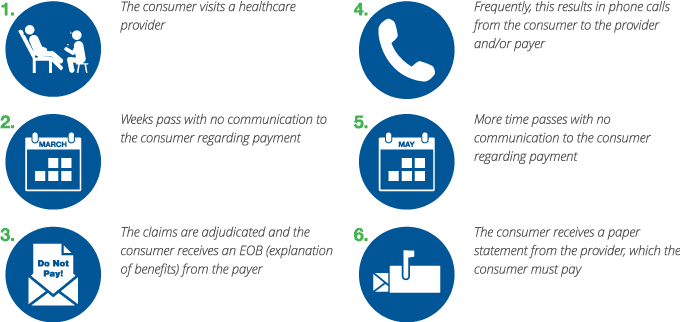
This common process is problematic for many reasons. First, so much time has passed since the initial provider visit that the consumer frequently has forgotten about the payment due. Consequently, the consumer commonly disregards this first statement. Furthermore, the payment options available to the consumer often are limited. The impacts to payers and providers include consumer nonpayment, high call volume and, most importantly, consumer confusion and dissatisfaction. Payers have the opportunity to collaborate with providers to improve this process and the consumer payment experience in healthcare payments.
Opportunities for Payers
Payers have a unique opportunity in this process because they manage the first communication (the EOB) with the consumer. Payers are able to improve the communication regarding payment responsibility and allow consumers to make a payment as soon as they understand their payment responsibility. The value of these opportunities to payers is to enhance the way they engage with their consumers and improve the consumer’s experience.
Best Practices
Payers can enable consumers to simplify their healthcare finances by integrating payment functionality within their member portals – for both premium and provider payments. As a best practice, payers should enable consumers to view payments owed to all providers across multiple family members, use their preferred payment method, securely save payment information for future payments and view how payments affect their deductibles, all in one place. Payers also can simplify the payment experience by supporting consumer-centric features such as mobile and tablet support and email communications for balance information and payment receipts.
Download the InstaMed white paper, Challenges and Opportunities for Payers in the Changing Healthcare Payments Landscape, to explore additional challenges and opportunities, and discusses the risks, best practices and topics for consideration for payers as they evolve their processes, policies and offerings to accommodate for the changing industry.
